I was a little underwhelmed with the overall quality of evidence in the GW presentations at TDO, with many cases shown as process-outcomes in cotton/cavit and no followup. That said, I'm not expecting five year followups from clinician who have had the device for 18 months, but from an evidential standpoint, presenting cases in setting sealer/cotton/cavit is…well…part of the problem that has plagued our specialty for decades and misled generations of clinicians.
That said, there were a couple of clinicians that showed mostly, or pretty much all cases with followup (as a side-note, one of those clinicians (Palermo) restores 100% of his cases…maybe there is some sort of relationship there between restorative and followups that the cotton/cavit crowd might take notice of 😀…).
The inference was made by many as to "early healing" with some 3-6 month followups which many have been doing for years now to assess treatment response as discussed on TDO, elsewhere and in the CBCT text (i.e. part of IGT), so this is no surprise, and something that happens routinely without GW, so the inference that GW is responsible for the improved biologic outcome is problematic at best.
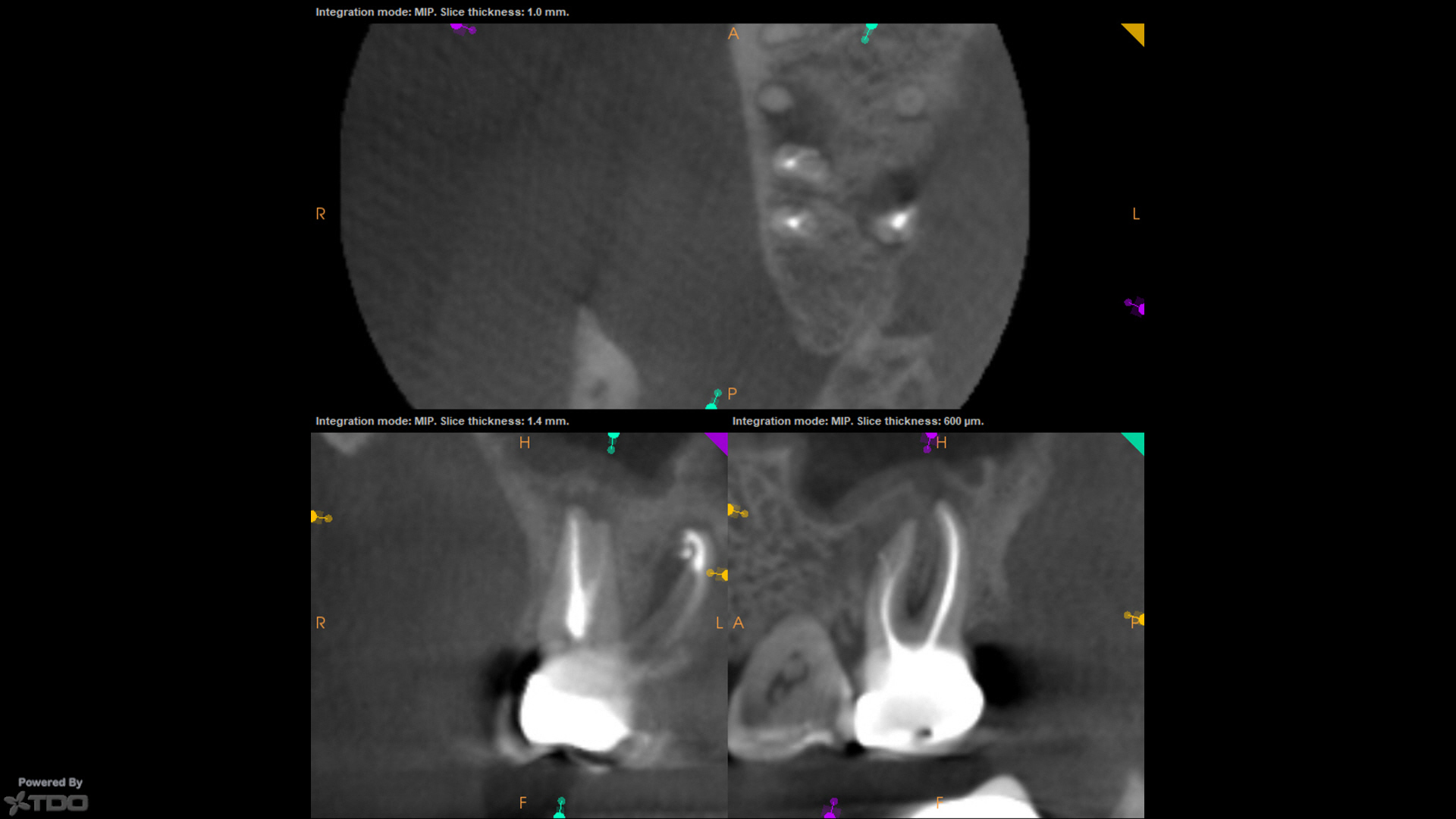
Process-outcomes were highly touted, many shown in setting sealer, some with CBCT, like this case from today (now yesterday), and then the inference made that those process-outcomes were a function of the GW.
As this now-asymptomatic case from today (now yesterday) shows, that also is not the case.
From the interim CBCT, I knew we had a deep split and separate MB2 POE. I obturated the MB canal with BC Sealer and a single cone, making no effort to do anything with the MB2 from a "cleaning and shaping and obturation standpoint." No downpack was performed. CBCT demonstrates at least something in MB2, as well as a lateral canal off-to-the-mesial. No GW was used.
I think claiming some sort of victory here is misleading at best, and attributing the process-outcome to some trick intervention parameter is…well…I'll wait for the followup…
What David and I have found is that by-and-large, most maxillary molars surviving at 20+ years don't have evidence of an MB2, or there is no evidence that it was found…and then the inference that the MB2 was missed, which is quite likely.
This brings-to-bear the importance of dealing with these things claimed to influence outcome over other issues, like simply doing the restorative (like Palermo showed). It's certainly important in some cases, but by throwing all patients into the GW arm, we'll never learn those things. This is what I found most disappointing. This also results in over-treatment of those patients with increased cost, and increased risk…discussion of which was…perhaps a little lacking???
From memory:
One of the presenters showed a GW case that didn't work, was addressed surgically, and then had followup.
Another presenter showed a case or two with GW that remained symptomatic, was treated with CH, and symptoms resolved.
I found this particular presenter to be the most careful in his thinking and management.
One presenter claimed 1200 single-visit GW cases and noted three failures, which greatly strains the credibility of other claims made in my eyes. That is, at 99% success, there should be 12 failures. Troubling to say the least.
As-a-group, the presenting clinicians put all of their patients in the GW arm with no comparator group. This is problematic for many reasons, and likely to lead to confident, incorrect inferences that have been rife in our specialty. This is what was done with Sonendo's "outcome study" in the JOE a bit back that was registered with about 120 patients, ended with about 70, and reported about 45…what happened to all those other patients???
What I was hoping to see is a multi-visit case like this patient in today with the maxillary bicuspid. There is clear and compelling radiographic evidence of resolution of AP, yet slight symptoms still remain. What I would like to see is a case like this, then GW was used, and the symptoms resolved, and a six-month followup. With six clinicians with thousands of cases, I would have liked to see something like this…actually…expected to see several cases like this.
By-and-large, I found those same kinds of inferential errors attributing whatever kind of outcome one wants to measure to the intervention, with no comparator group, and likely dominated by an occult prior probability. That is…if you have/had been taking short-term CBCTs to evaluate treatment response, and taking post-ops with CBCT, you would be seeing the kinds of things that have been claimed as a function of the GW, when they have/had been occurring all-along…if they even mattered anyways.
All that said, some of the process outcomes…speaking as an endodontist that likes cool-looking cases as much as the next guy, were quite impressive…but as Dr. Lewis says: "Don't confuse that with outcomes!"
The thing is, we have been here in endodontics so many times before.
I remember Osama Ben Schein quoting me back to me from my single-visit days: "If it gets a rubber dam, it get's gutta-percha" back in the "rotary-revolution-single-visit-endo" days. I signed on to TDO over a dozen years ago, saw Gary doing the most difficult and problematic of cases with followup…cases that I had and had trouble with in my practice and it didn't take long to make the switch to multi-visit. There is a way to demonstrate efficacy with even just a handful of cases, unfortunately, throwing everyone into the GW arm and claiming whatever success isn't it.
There is good evidence that the device does what the manufacturer says it does at the benchtop. There are reasons to believe it does that in-vivo as well. However, I find the evidence for translation to improved biologic, or patient-centered outcomes lacking…and I was really hoping to be convinced otherwise, as these multi-visit cases, like this refractory one in today…are a nuisance to everyone.
I would gladly pay $65K + $100/pop to quit doing multi-visit endo.
I was hoping for some better evidence…but not really expecting it anymore.
Subscribe
Login
Please login to comment
0 Comments